

Diabetes And Magnesium: The Emerging Role Of Oral Magnesium Supplementation
The link between diabetes mellitus and magnesium deficiency is well known.
A growing body of evidence suggests that magnesium plays a pivotal role in reducing cardiovascular risks and may be involved in the pathogenesis of diabetes itself.
While the benefits of oral magnesium supplementation on glycemic control have yet to be demonstrated in patients, magnesium supplementation has been shown to improve insulin sensitivity. Based on current knowledge, clinicians have good reason to believe that magnesium repletion may play a role in delaying type 2 diabetes onset and potentially in warding off its devastating complications — cardiovascular disease, retinopathy, and nephropathy.
Magnesium needs in the American population
The Recommended Daily Allowance (RDA) for magnesium is 6 mg/kg/d. This means 400 mg/d to 420 mg/d for adult men and 320 mg/d for adult women (and even more for women who are pregnant or lactating). By these standards, which have been promulgated by the National Academy of Sciences and the Institute of Medicine after great deliberation, research, and literature review, an estimated 50% to 85% of the population of the United States is receiving an inadequate magnesium intake.
Levels of magnesium may be particularly low in certain populations, such as African Americans. For example, the prevalence of hypomagnesemia is 20% among urban African Americans in the city of Buffalo, NY, and surrounding area. This exceeds the prevalence of hypomagnesemia in the general population, and implies a risk for diabetes, hyperlipidemia, hypertension, other cardiovascular disease, and renal disease. Low dietary magnesium intake is correlated with insulin resistance in non-elderly African Americans without diabetes.
The American Diabetes Association (ADA) recognizes the increased risks associated with magnesium deficiency in patients with certain diseases or conditions (Table 1). In addition, the ADA recommends that magnesium levels be measured in such patients and repleted if deficient.
Magnesium levels in patients with diabetes
Many studies have shown that both mean plasma and intracellular free magnesium levels are lower in patients with diabetes than in the general population. This magnesium deficiency, which may take the form of a chronic latent magnesium deficit rather than clinical hypomagnesemia, may have clinical importance because the magnesium ion is a crucial cofactor for many enzymatic reactions involved in metabolic processes.
Many studies show that mean plasma levels are lower in patients with both type 1 and type 2 diabetes compared with non-diabetic control subjects. The concentration of intracellular free magnesium in erythrocytes is a more sensitive marker in people with diabetes and insulin resistance than are plasma levels of magnesium. Decreased levels of free intracellular magnesium in erythrocytes have been reported in the majority of patients with type 2 diabetes.
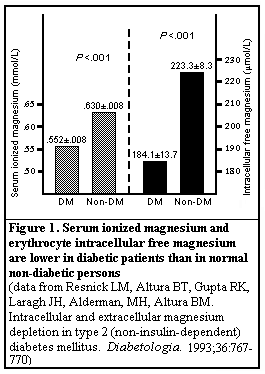
Resnick and associates suggest that extracellular and intracellular magnesium deficiency is typical in chronic, stable, mild type 2 diabetes and may be a strong predisposing factor for the development of the excess cardiovascular morbidity associated with diabetes. These investigators showed that the levels of serum ionized magnesium and erythrocyte intracellular free magnesium were significantly lower in 22 untreated patients with type 2 diabetes and mild hyperglycemia than they were in 30 healthy control subjects (P<.001) (Figure 1). Serum total magnesium was not reduced.
Table 1. ADA Recommendations for Magnesium Measurement |
According to the ADA, serum magnesium levels should be measured in patients who have diabetes with these concomitant conditions:
|
Magnesium loss and insulin resistance
Among its many actions, insulin stimulates the transport of magnesium from the extra-cellular to the intracellular compartment. Using atomic absorption spectrophotometry and the euglycemic hyperinsulinemic glucose clamp technique, Paolisso and associates showed that plasma magnesium level declined and erythrocyte magnesium levels rose significantly (P<.05) in response to insulin in fasting healthy adults with no family history of diabetes.
Insulin resistance — central to type 2 diabetes — is associated with reduced intracellular magnesium and can be mitigated with magnesium. It has been demonstrated that insulin resistance in skeletal muscle can be reduced by magnesium administration.
Reduced magnesium levels in diabetes are caused by several factors (Table 2). The link between magnesium deficiency and the development of diabetes is strengthened by the observation that several treatments for type 2 diabetes appear to increase magnesium levels. Metformin, for example, raises magnesium levels in the liver. Pioglitazone, a thiazolidinedione antidiabetic agent that increases insulin sensitivity, increases free magnesium concentration in adipocytes.
Table 2. Reasons for Low Magnesium Status in Diabetes |
|
Clinical implications of low magnesium levels
Magnesium deficiency is associated with insulin resistance and increased platelet reactivity, but studies of oral magnesium supplementation and changes in glycemic status or lipid levels in diabetes have not been conclusive. When my colleagues and I gave oral magnesium to 20 patients with type 2 diabetes, intracellular free magnesium concentration in erythrocytes normalized and the increase in platelet reactivity in response to thromboxanes decreased significantly. The oral dosage was 400 mg / d of elemental magnesium.
Shortly thereafter, we reported that infusing magnesium into healthy subjects reduced urinary thromboxane concentration and angiotensin II-induced plasma aldosterone levels; conversely, dietary induced magnesium deficiency led to increased thromboxane and aldosterone synthesis and decreased insulin sensitivity. Just this year, Rosolová and colleagues confirmed that magnesium deficiency decreases insulin-mediated glucose disposal in non-diabetic subjects, which is consistent with insulin resistance. There is, however, no consistent evidence supporting a direct effect of magnesium intake on glycemic control.
Reduced intake and reduced levels of magnesium may lead to increased atherosclerosis. In addition, lower serum magnesium levels have been associated with increased likelihood or progression of retinopathy in type 1 and type 2 diabetes.
Epidemiologic data suggest that populations with low magnesium intake are at increased risk for hypertension, stroke, and other manifestations of atherosclerotic disease. In the Atherosclerosis Risk in Communities (ARIC) Study, for example, dietary magnesium intake was inversely correlated with ultrasonographically measured carotid artery wall thickness, which is a surrogate marker for atherosclerosis.
Oral magnesium: Value of a high intake
There are potential benefits supporting the use of magnesium supplementation in persons who have diabetes or risk factors for diabetes (Table 3). Increased magnesium intake is associated with decreased risk of developing type 2 diabetes in populations. In a prospective study of almost 85,000 women, the relative risk of diabetes for women in the highest quintile of magnesium consumption was 0.68 when compared with women in the lowest quintile (Figure 2). Oral magnesium supplementation is contraindicated in patients with significant renal impairment.
Table 3. Rationale for Oral Magnesium Supplementation in Diabetes |
Magnesium supplementation does the following:
|
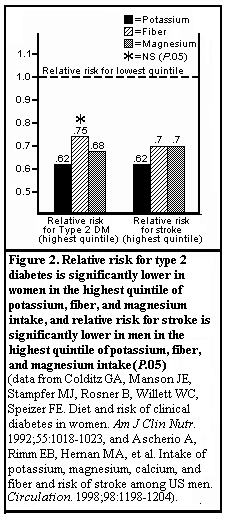
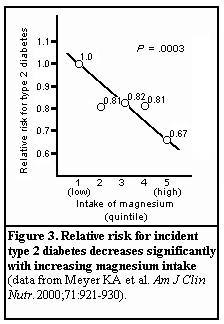
Higher dietary intake of magnesium was among the factors associated with a reduced risk of stroke in men with hypertension. In a survey of almost 45,000 men ages 40 to 75, the overall risk of stroke was significantly lower for men in the highest quintile of intake of potassium, magnesium, and cereal fiber, but not of calcium, compared with men in the lowest quintile of intake (Figure 2). A similar relationship was reported this year by Meyer and colleagues, who observed that a diet rich in magnesium, grains, fruits, and vegetables reduced the likelihood of developing type 2 diabetes in a group of almost 36,000 women (Figure 3). While no consistent effect of magnesium on blood pressure has been noted among persons with diabetes, a significant blood pressure reduction was noted in diabetic patients with hypertension after dietary sodium was replaced with potassium and magnesium.
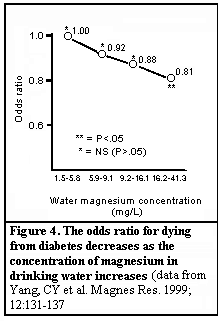
In a study from Taiwan, the risk of dying from diabetes was inversely proportional to the level of magnesium in the drinking water (Figure 4). This was all the more striking because the greatest increase in chronic disease mortality in Taiwan since 1970 has been due to diabetes. Because the dysregulation caused by a chronic latent magnesium deficit is probably more important than clinical hypomagnesemia in the pathogenesis of diabetes, this may suggest that dietary magnesium (including that in a water supply) is protective against diabetes and its dreaded complications.
Citations:
De Valk HW, Magnesium in diabetes mellitus. Neth J Med. 1999;54:139-146.
Ewis SA, Abdel-Rahman MS. Influence of atenolol and / or metformin on glutathione and magnesium levels in diabetic rats. J Appl Toxicol. 1997;17:409-413.
Fox CH, Ramsoomair D, Mahoney MC, Carter C, Young B, Graham R. An investigation of hypomagnesemia among ambulatory urban African Americans. J Fam Pract. 1999;48:636-639.
Humphries S, Kushner H, Falkner B. Low dietary magnesium is associated with insulin resistance in a sample of young, nondiabetic Black Americans. Am J Hypertens. 1999;12(8 Pt 1):747-756.
Kao, WH, Folsom, AR, Nieto FJ, Mo JP, Watson RI, Brancati FL. Serum and dietary magnesium and the risk for type 2 diabetes mellitus: the Atherosclerosis Risk in Communities Study. Arch Intern Med. 1999;159:2151-2159.
Meyer KA, Kushi LH, Jacobs DR Jr, Slavin J, Sellers TA, Folsom AR. Carbohydrates, dietary fiber, and incident type 2 diabetes in older women. Am J Clin Nutr. 2000;71:921-930.
Nadler JL, Buchanan T, Natarajan R, Antonipillai I, Bergman R, Rude R. Magnesium deficiency produces insulin resistance and increased thromboxane synthesis. Hypertension, 1993;21(6 Pt 2):1024-1029.
Nadler JL, Malayan S, Luong H, Shaw S, Natarajan RD, Rude RK. Intracellular free magnesium deficiency plays a key role in increased platelet reactivity in type II diabetes mellitus. Diabetes Care. 1992;15:835-841.
Nadler J, Scott S. Evidence that pioglitazone increases intracellular free magnesium concentration in freshly isolated rat adipocytes. Biochem Biophys Res Commun. 1994;202:416-421.
Paolisso G, Sgambato S, Pizza G, Passariello N, Varricchio M, D’Onofrio F. Improved insulin response and action by chronic magnesium administration in aged NIDDM subjects. Diabetes Care. 1989;12:262-269.
Rosolová H, Mayer O Jr, Reaven GM. Insulin-mediated glucose disposal is decreased in normal subjects with relatively low plasma magnesium concentrations. Metabolism. 2000;49:418-420.
Sasaki S, Oshima T, Matsuura H, et al. Abnormal magnesium status in patients with cardiovascular diseases. Clin Sci (Colch). 2000;98:175-181.
Yang CY, Chiu HF, Cheng MF, Tsai SS, Hung CF, Tseng YT. Magnesium in drinking water and the risk of death from diabetes mellitus. Magnes Res. 1999;12:131-137.


